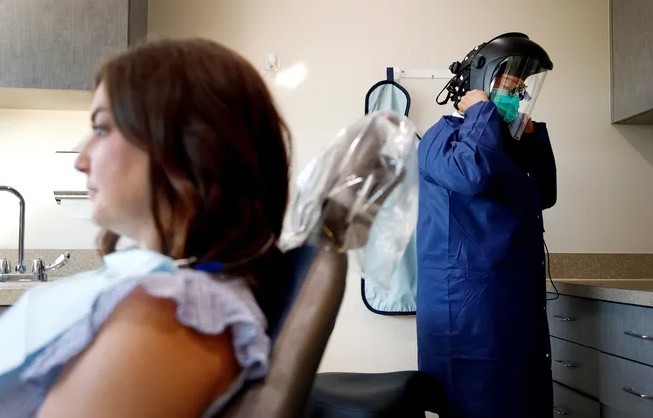
Dentists and orthodontists reopening across metro Detroit have been making big investments in protective gear, technology and equipment as they work to make sure patients and staff are protected from COVID-19.
But the changes, which can vary greatly by office, are not all required and are being done at the discretion of each dentist and orthodontist, raising the question of what risks you face at your next appointment and what you need to know before you go in.
Closed lobbies, virtual paperwork, tele-health appointments, fewer patients and protective gear like disposable gowns, masks, shields and gloves are common changes among some metro Detroit dentists and orthodontists. Others have gone beyond that, adding higher-tech improvements like aerosol remediation devices and air purifiers that better filter the particles that come out of our mouths that put us at risk for catching COVID-19.
Advocates say patients and dental staff need to understand that until the coronavirus is fully understood, most of the changes dentists are making are based on state and national recommendations using the latest information available.
Plus, with varied levels of virus exposure, it has been difficult for state associations to mandate protective equipment, especially when there were initial shortages of items such as N95 masks — which went to hospitals before they went to dentists, said Dr. Steve Meraw, a periodontist and president of the Okemos-based Michigan Dental Association.
As a result, experts agree, patients need to understand the equipment, the potential hazards and what kind of questions they should ask before a visit.
Not all the same
At Caring Smiles Family Dentistry in West Bloomfield, partners and spouses Dr. Warren Woodruff and Dr. Amira May Woodruff,installed a medical-grade air purification system in each of their treatment rooms to better filter particles that could be emitted from patients’ mouths during procedures. Those aerosols can travel or linger in the air.
The Woodruffs also purchased additional protective gear, including face shields, and ditched their lab coats for scrubs and disposable gowns, gloves and masks.
They change their masks between patients and change gowns if they become visibly soiled, following MDA and American Dental Association recommendations, Amira May Woodruff said.
“Since the beginning of time, dentistry has been an intimate, close environment. For many years, our profession has been exquisite when it comes to infection control. That’s our forte,” said Amira May Woodruff. “Yes, coronavirus is new and scary. But the dental office is not a place to be scared of. We’ve got it covered.”
Dentist and orthodontist practices in Michigan had to close in mid-March as non-essential medical offices during the state’s quarantine. Gov. Gretchen Whitmer allowed the industries to reopenMay 29, but the rebound, while steady, has been slow, surveys show.
The American Dental Association has done a weekly poll of its members, including those in Michigan, since the coronavirus began to impact its membership. Its June 15 poll had 33.8% of dental offices nationwide reporting they were open with business as usual; 62.9% reported they are open but with lower patient volume than usual. In Michigan, 40.5% reported business as usual and 58.1% said there was lower patient volume.
Dr. Chad Gehani, president of the ADA, said the organization has been focusing on guidance rather than mandates at this early stage.
“The ADA is a voluntary membership organization and not a regulatory body, and as such does not issue mandates. The ADA’s guidance has been widely available for use during the pandemic to member and non-member dental teams,” Gehani said.
He added: “The guidance includes specific recommendations before, during and after dental appointments, as well as recommendations for pre-screening patients and staff, supplies shopping list and staff and patient protection strategies.”
In addition to the ADA’s template for going back to work, Michigan’s Licensing and Regulatory Affairs (LARA) office also provided a four-page guidance sheet for outpatient dental practices to safely restart, said the MDA’s Meraw.
“Early on, Michigan was more of a hot spot, so we wanted to be very cautious,” Meraw said. But it’s “hard to put one mandate down for everybody,” when the number of cases vary greatly in different parts of the state, he said.
One early struggle was the industry’s concern over receiving enough Personal Protection Equipment or PPE, such as N95 masks, which are necessary for certain dental procedures, such as those that give off extra potential splatter. During the height of the pandemic, the MDA had asked its members to donate PPE to hospital and medical staff because it was the right thing to do, Meraw said.
Now, MDA works with other professional associations, including the ADA and the Detroit District Dental Society to secure PPE for distribution to members.
“As we reopened, (dental practices) became a higher priority, so we started getting more PPE and we’re really starting to catch up on all of it,” Meraw said, noting that some of his delayed orders for masks and touchless thermometers are still arriving weeks after ordering them. “The supply chain is improving, so we’re cautiously optimistic that we will continue to get access to (the PPE) we need.“
At Doolin Haddad Advanced Dentistry in Rochester, Dr. Jeff Haddad said masks and gowns are changed between patients and he now stocks three types of masks, including KN95s (masks made in other countries under different standards), for high-contact procedures.
“Unfortunately, it was nearly impossible for any dentists to obtain N95 masks throughout this pandemic,” Haddad said, so he sought out the KN95. “(KN95s) are on the FDA approved list. This is still over and beyond what most dentists are using because of the high expense of KN95 masks and the scarcity of them.”
He does more virtual consultations so potential patients don’t have to come into the office. He also installed an office-wide surgically clean air filtration system, designed to capture microbial pollutants and toxins. It also kills airborne viruses while improving the office’s overall air quality, Haddad said.
“We were doing everything very well but we wanted to take it to the next level, not only from a safety standpoint but a health standpoint,” Haddad said. “I had considered (this system) before, but right after the shutdown I made a phone call and had it within a week. … You notice a difference in the air. This is something I wish I had done sooner.”
A heavy responsibility
Under those masks and face shields, dentists and orthodontists say they are still smiling, but the responsibilities and weight of their everyday decisions is much larger now.
“We’re at half capacity since we reopened,” going from about 120 patients per day to around 60, said Dr. G. Michael Kabot, an orthodontist with offices in Clawson and Farmington Hills.
Kabot, who added air purifiers, ion generators and acrylic shields between stations to prepare for patients and his staff returning, said staff change masks between each patient but only change gowns if certain procedures have been done, such as those that create aerosols. If it is a simple check on a retainer, which does not tend to release aerosols, they keep the gowns on, Kabot said.
To contain aerosols, Kabot said he created a special, separate area within his offices to maintain extra space between those procedures and the rest of the treatment areas. He also is limiting how much water he uses in high-speed drilling, something he started a while back, which creates fewer aerosols, as well.
Dr. William S. Demray at Preservation Dental in Northville added an aerosol remediation device, which helps with droplet capture from patients. Before reopening June 1, there was an orientation day with the entire staff to introduce the new devices and answer any questions they might have about returning.
Demray knew some hygienists nationwide were worried about returning to work, and he said he wanted his staff to feel safe and informed.
“We spent about a month perfecting it during the downtime so it was ready to use when we got back into the office,” Demray said. “We wanted to remove (aerosols) at the source — we’re trying to make sure our viral load is at the absolute minimum.”
More:After Michigan flattened the curve, coronavirus case counts appear to be rising
Holly-based dentist Dawn Kulongowski, who owns Creative Smiles Dental Group, said she understands the patient’s point of view in a unique way given her personal concerns about viruses. She closed her dental office after her last patient on March 12 and began rethinking her protocols and procedures.
“We have infection control down. We know what we’re doing,” Kulongowski said.
In addition to requiring masks, daily health screenings for staff and patients and limited guest access to the office, Kulongowski added surgical air filters through the office – which will clean the entire office’s air about every 8 minutes and filter down to 0.1 micron.
She added specialized suction devices at each treatment area. She also mists each treatment room between patients with HOCl or hypochlorous acid, which is a powerful and safe disinfectant made from electrolyzed salt water.
Kulongowski, who said she has worn a shield the last 18 years of her 20 years as a dentist, said she had thought ahead on the need for N95 masks and related PPE. As a result, she had a good supply in place when she reopened.
Her office also changes gloves and gowns between every patient.
Still, the changes and new procedures made that first week or two on the job tiring, she said. “It was stressful at first; I cannot lie about that,” Kulongowski said. “By the end of the shutdown, I started to feel like I was neglecting patients.”
One of her patients, Kathryn Sharbaugh, came to see Kulongowski twice – once during the quarantine on an emergency basis and once for a follow-up visit during regular hours. Sharbaugh, 72, of Holly, was in quarantine with her 75-year-old husband, but she had an abscess that she wanted Kulongowski to see, Sharbaugh said.
Kulongowski had to refer Sharbaugh to an endodontist, but she kept track of Sharbaugh, her care and her response to treatment. These days, Sharbaugh said she is feeling fine but knows that not every dentist or dental professional is like Kulongowski.
“I felt so safe and so cared for when I was there,” Sharbaugh said.
What to ask
Dental and orthodontic practices have changed since reopening in May. Here are some questions you can ask to see what kind of health and safety improvements your dentist or orthodontist have made:
- How are you minimizing potential harm to patients from possible exposure to the coronavirus?
- What is your screening process for employees and patients to enter the facility?
- How are you managing the lobby, patient treatment areas and public spaces?
- What are your cleaning, disinfecting and sanitizing routines for equipment?
- What kind of PPE are you providing for your employees?
- How are you working with patients and personnel to stay home if someone is sick?
Source: Michigan Dental Association, American Dental Association


